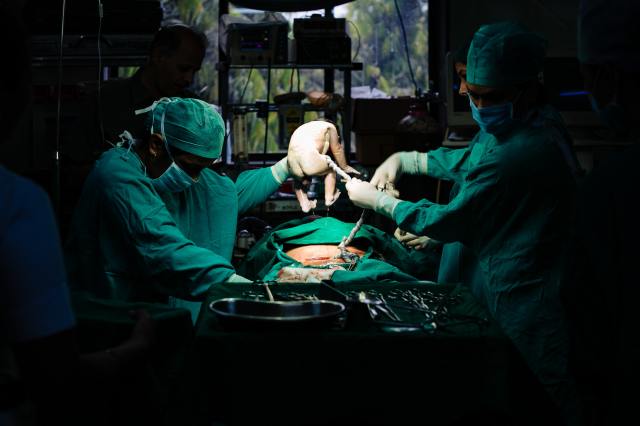
In the United States, approximately one-third of all babies are delivered by cesarean section. Many pregnant women have questions about C-section safety and frequency and wonder if they will need to undergo the procedure themselves. Here are some of the most common questions and concerns expectant mothers have about C-sections.
1. What is the rate of C-section births in the United States?
The Centers for Disease Control and Prevention report that more than 31% of U.S. deliveries were by C-section in 2018. Alabama, Louisiana, and Florida have the highest C-section rates, while Idaho, Utah, and Nevada have the lowest. C-sections are the most common surgery in the United States.
Few people are aware of this—and many of these C-sections are unnecessary. In fact, the number can be safely reduced to less than 15%, and for those women with low-risk pregnancies, reduced to 11%. When I joined my first practice after residency, the C-section rate in that group was 15%, which I regarded as too high. My C-section rate in my residency had been 10.9%. Working with the clinic staff, we safely reduced the C-section rate to 10% by offering women vaginal birth after cesarean section (VBAC), delivering breech babies vaginally, and using appropriate labor management treatment for dysfunctional labor and fetal distress.
2. Why is the C-section rate so high in the United States?
The rate is high for many reasons, a number of them unfortunate. For example, the use of fetal monitoring during labor and delivery has increased the C-section rate. The intent of the monitoring is to increase the baby’s Apgar score during labor and delivery, but it doesn’t. It just increases the C-section rate. A baby’s heart rate may decelerate after a contraction, and this is considered a sign of distress. This triggers the notion that a C-section is needed because the baby is in distress. The problem is that there is no way to know why the baby is in distress, and hence whether the baby needs to be delivered immediately. Fetal scalp blood samples can be taken, but this delays the C-section if needed.
There is no doubt some C-sections are done to save time. If you know what you’re doing, C-sections take 20-to-30 minutes. Inductions can take hours, as can natural labor. Add to that the fact that insurance companies pay about twice as much for a C-section as for an induced or natural delivery, and it’s easy to see why the procedure is so popular.
3. What are the risks involved with having a C-section?
With a C-section, the two highest risks are infection of the tube that connects the kidney to the bladder, and hemorrhage. Infection occurs in 6 – 11% of C-sections. Bladder or ureter injury is also a high risk with this procedure. These injuries can often be repaired by the surgeon doing the C-section, but the long-term effects of failure to recognize this condition are bothersome.
4. What questions should I ask the obstetrician or surgeon doing my C-section?
The time to ask questions is before the need to have a C-section, during a prenatal visit. Your physician should be able to tell you their C-section rate as well as whether or not they have performed any C-hysterectomies. It’s also important to ask what the hospital’s C-section rate is. Hospitals vary widely in the number of C-sections performed. If you really want to avoid the chance of a C-section for “failure to progress,” choose a physician who regularly delivers babies vaginally, choose to avoid inductions, and check your hospital’s C-section rate.
5. If I’ve had a C-section for a previous birth, will I still be able to have a vaginal birth with a later pregnancy?
In most cases, you may have a vaginal birth after C-section (VBAC) as long as your C-section incision is left to right rather than up and down. When I joined my first practice after residency, I began doing VBACs after one previous C-section. I then offered VBACs after two C-sections, even three C-sections. A nurse practitioner came to see me with four previous C-sections. She knew and understood her options, and wanted to try a VBAC. Her labor and delivery went fine. She delivered her fifth child vaginally with no problems. The patients simply need to be monitored carefully. Checking for uterine rupture is to be expected. In all the VBACs I have done, including with women who’d had multiple C-sections, I have never had a uterine rupture.
Be sure to take these questions and any others you may have to your own obstetric care provider before giving birth with them. It’s important to ensure that you and your doctor are aligned on your goals and wishes for delivery, and it is very wise to advocate for yourself and your baby before delivery.